39-year-old male with a past medical history significant for diabetes, diabetic proliferative retinopathy s/p endo-laser photocoagulation in bilateral eyes, known left ocular retinal detachment secondary to proliferative retinopathyy, past plantar vitrectomy,and stripping, GERD presenting to the ED as a stroke alert. Chief complaint of atraumatic vision loss in his left eye. Patient noted sudden onset of gradual vision loss within the last 24 hours that has continued to worsen by the morning of his presentation. He notes that he can only see flickers of light from the left eye without any motion or delineation of objects. He denies any additional focal neurological deficits including sensory or motor weakness, facial droop, speech difficulties. Denies any headache, trauma, recent travel or illness.
Vitals: B/P 138/88, Pulse 62, Resp. 20, Temp 98.7 °F (37.1 °C), SpO2 99%
Physical exam was significant for – Left eye vision – flickers of light visible only, unable to see finger counting. Snellen OD 20/25, OS >20/400. IOP left eye 19mmhg, right side 20mmhg. No cranial nerve palsies. Strength and sensation intact throughout. Normal gait and reflexes. No abnormal cardiac/lung sounds, normal pulses.
Clinical course
The stroke alert process was de-escalated as the patient had presented with an ocular complaint. No lab panel was obtained but a POC glucose was 125 mg/dl. Patient was sent for HCT and ocular US.
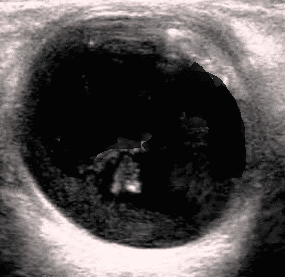
Bedside ultrasound of the left eye – displayed accumulation of swirling material in the aqueous humor with oculokinesis concerning for vitreous hemorrhage. No obvious retinal detachment.
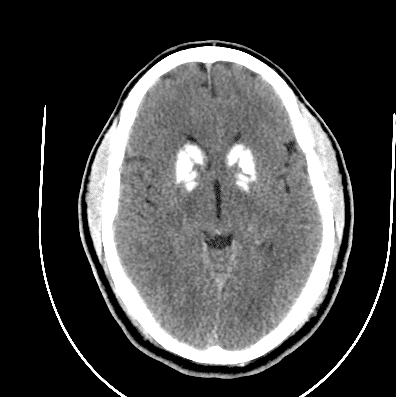
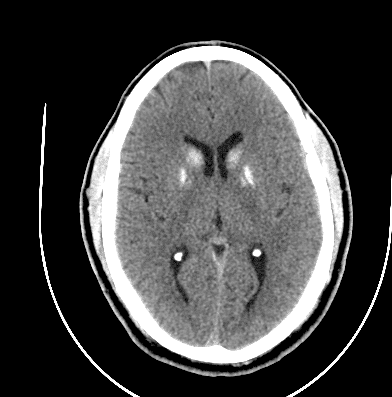
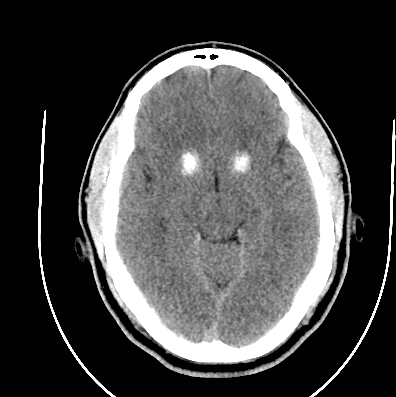
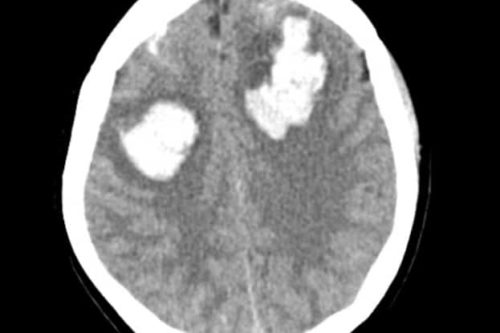
CT Head with Orbits wo contrast – Unremarkable CT of the orbits. Symmetric calcifications of the bilateral basal ganglia noted on the CT head.
Head CT Imaging

Ocular Ultrasound Imaging
Fahr Disease/Fahr Syndrome- Idiopathic basal ganglia calcification (IBGC)
Idiopathic basal ganglia calcification (IBGC), also known as bilateral striopallidodentate calcinosis, Fahr syndrome, or Fahr disease is a rare neurodegenerative condition characterized by the accumulation of calcium deposits in the basal ganglia and other brain regions, most easily visualized on computed tomography (CT) scan.
Several neurological signs and symptoms are associated with Fahr’s syndrome. In adults gait disorder, speech impairment, dementia, and coma have been seen. Loss of consciousness, tetany and seizures have been reported with associated hypothyroid hypocalcaemia (3,5,6). Papilledema of intracranial hypertension, Pleocytosis of CSF and paroxysmal Choreothetosis have also been reported. Symptoms characteristic of Parkinson’s disease can be found such as tremors, muscle rigidity, a mask-like facial appearance, shuffling gait, and a “pill-rolling” motion of the fingers. These symptoms generally occur later in the development of the disease. More common symptoms include dystonia (disordered muscle tone) and chorea (involuntary, rapid, jerky movements). Age of onset of symptoms is typically in the 40s or 50s, although it can occur at any time in childhood or adolescence. (1)
The sporadic (IBGC) and familial (Primary Familial Brain Calcification) forms of brain calcification are not associated with disorders of calcium or parathyroid hormone metabolism, such as hypoparathyroidism or pseudohypoparathyroidism. However, the localization of intracranial and basal ganglia calcification that can occur with hypoparathyroidism is similar to that seen in IBGC and PFBC.
Differential Diagnosis: Normal aging, CO2 poisoning, hypoparathyroidism, toxoplasmosis, rubella, brucellosis, cytomegalovirus, cysticercosis, AIDS/HIV, Wilson’s disease, Cockayne syndrome, tuberous sclerosis, and rarely Down’s syndrome. (6)
The prognosis for any individual with Fahr’s Syndrome is variable and hard to predict. There is no reliable correlation between age, extent of calcium deposits in the brain, and neurological deficit. Diagnosis is difficult and may be easily confused with other conditions. Treatment thus far revolves around addressing neuropsychiatric symptoms with benzos or atypical antipsychotics, oxybutinin for incontinence, and treatment of hypoparathyroidism. (7,8,9)
Case discussion
The vitreous hemorrhage was found to be related to the patient’s diabteic retinoproliferative disease and not related to the Fahrs syndrome which was discovered incidentally. The patient underwent Ophthalmology consultation with planned outpatient laser surgery and outpatient neurology referral for MRI, EMG testing, and further genetic workup. No additional medications were prescribed on discharge.
References
- da Silva RJ, Pereira IC, Oliveira JR: Analysis of Gene Expression Pattern and Neuroanatomical Correlates for SLC20A2 (PiT-2) Shows a Molecular Network with Potential Impact in Idiopathic Basal Ganglia Calcification (“Fahr’s Disease”). J of Molec Neuro: MN. 2013, 50 (2): 280-283. 10.1007/s12031-013-0001-0.
- Manyam BV, Walters AS, Narla KR: Bilateral striopallidodentate calcinosis: clinical characteristics of patients seen in a registry. Movement disorders: official journal of the Movement Disorder Society. 2001, 16 (2): 258-264. 10.1002/mds.1049.
- Arranz PM, Ergueta MP, González SE, Marañón CA: Fahr’s disease and hypocalcemic syndromes. Presentation of a clinical case. Anales de medicina interna. 1992, (Madrid, Spain, 1992-495.
- http://www.ncbi.nlm.nih.gov/pubmed/1420763.
- Lauterbach EC, Spears TE, Prewett MJ, Price ST, Jackson JG, Kirsh AD: Neuropsychiatric disorders, myoclonus, and dystonia in calcification of basal ganglia pathways. Biol Psychiatry. 1994, 35 (5): 345-351. 10.1016/0006-3223(94)90038-8.
- Arias MJ, González MT, Escorial MC, Marañón CA: Intracranial calcifications in the differential diagnosis of epileptic disease]. Rev Clin Esp. 1991, 189 (9): 425.
- Sobrid SH MJ, Geschwind DH: Familial Idiopathic Basal Ganglia Calcification: GeneReviews™ [Internet]. Seattle (WA): University of Washington, Seattle; 2004. Updated 2007 Sep 20.
- el Maghraoui A, Birouk N, Zaim A, Slassi I, Yahyaoui M, Chkili T: Fahr syndrome and dysparathyroidism. 3 cases. Presse Medicale Paris, France: 1983. 1995, 24 (28): 1301-1304.
- Abubakar SA, Saidu S: Idiopathic bilateral strio-pallido-dentate calcinosis (Fahr’s disease): a case report and review of the literature. Ann Afr Med. 2012, 11 (4): 234-237. 10.4103/1596-3519.102855.
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3960784/

This Post Has 0 Comments