Clinical Case Study
You are on ICU and called to the floor for respiratory distress, respiratory rate 50s, despite being on CPAP. You send your intern to evaluate while you chart review to find out:
63yoF PMH of HTN, autoimmune hepatitis c/b cirrhosis w/ esophageal varices s/p TIPS, admitted 7 days ago for sepsis 2/2 RUL pna. She completed 7 days of appropriate abx, and received IVF boluses. Net +7L since admission. Unknown family history, former 5 pack years smoker. Meds: lactulose, rifaximin, coreg for HTN . ROS: SOB, chronic leg swelling. Denies cough, CP, fevers, chills, AP, abdominal distention, n, v.
You join your intern to see the patient…
VS: afeb, HR 117, RR 50, BP 133/75, CPAP 50% 7 cm H2O, sat 94%
She appears to be in distress but A&Ox4. Tachypnic with shallow breathing on CPAP. Transmitted upper airway noises on auscultation but you hear b/l rales and rhonchi R>L. She is tachycardic but with regular rhythm. Normal S1,S2. JVD indeterminate due to body habitus. 1+ non-pitting edema bilaterally. With no TTP.
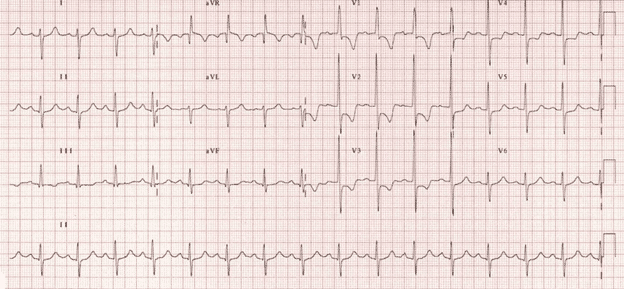
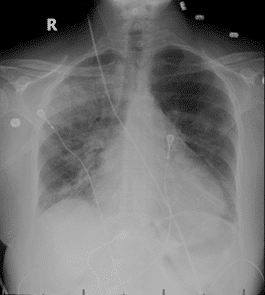
You order a stat CXR and EKG (see below)
Now the EKG

You see sinus tachycardia, rate around 100. You notice S1, T3. Some ST/Twave changes in the anterior leads
DDx: Consider PE, ARDS, pna, ILD, valve rupture, intracardiac shunt, pHTN
Pt appeared fluid overloaded and placed on lasix drip. Pt is stabilized and you obtained CT PE protocol and ECHO
ICU course…
Repeat CTA PE protocol returns negative for PE and shows resolving RUL infiltrate but worsening b/l groundglass opacities. Edema vs infectious. Worsening cardiomegaly when compared to prior CT this admission. ECHO showed EF 60-65%. Impaired diastolic filling. Severely enlarged RV. Moderate TR. Severely elevated pulmonary artery systolic pressure. Cardiology consulted for RHC which showed severe pulmonary hypertension and elevated right sided filling pressures (RVSP at 70 mmHg). PCWP noted to be 6 mmHg. Now you are thinking something is straining your patient’s right heart, but you know from the RHC it’s not the left side of the heart so it has to be somewhere in between…the LUNGS!
Given pt’s history of autoimmune hepatitis, you and Cardiology suspect pulmonary HTN, specifically portopulmonary HTN (WHO Class 1). This patient likely has acute worsening of her chronic pressures secondary to her severe acute pulmonary disease (PNA vs ARDS vs Pulmonary edema).

The prevalence of Pulmonary Hypertension (pHTN) is 2-16% in End-stage liver disease (ESLD) portal HTN; aka portopulmonary HTN. Unknown pathogenesis, but theories involving: imbalance of vasoconstrictive and vasodilatory mediators (ESLD, so liver unable to metabolize), genetic predisposition, thromboembolism from the portal venous system, Inflammation related to ESLD1.
pHTN Basics1,2,3
- Severity (mean PAP)
- Normal is 12-16 mmHg
- Mild = 25-40mmHg
- Moderate = 41-55mmHg
- Severe = > 55mmHg
- Exam: increased JVP, parasternal heave, TR murmur, hepatomegaly,
- Goals of mgmt: optimize PAP, RV preload, avoid RV ischemia
- O2, bronchodialators, vasodilators, inotropes
- inhaled nitric oxide, milrinone, dipyridamole, inhaled/IV prostacyclin, RV assist device
- Intubation last resort!
Unfortunately, despite your best efforts utilizing many of the components of the above strategy, pt was eventually intubated, required increasing doses of vasopressors and mechanical ventilatory support. Unable to wean from vent and family decided to move to comfort care.
Although not sensitive, EKGs can have clues suggesting cor pulmonale, any primary pulmonary process that causes functional or structural changes on the heart (right heart because it is downstream). Let’s discuss what we can find for acute and chronic heart strain!
pHTN may have normal EKG, but you may find signs of4:
- RVH
- p-pulmonale/RAE
- RAD
- tall R waves in V1
- right ventricular strain
RVH is a structural change to the R side of heart and is a chronic process. In addition to pHTN, you can also see it in mitral stenosis, pulmonary stenosis, congenital heart diseases (TOF).
- Diagnostic criteria for RVH5
- QRS duration < 120 ms.
- Right axis deviation > +110°
- Dominant R wave in lead V1 ⩾7 mm
- Supporting criteria for RVH5
- ST segment depression/T wave inversion in anterior/inferior leads
- Aka acute heart strain that we will discuss later
- Deep S waves in leads V5, V6, I, and aVL (clockwise rotation)
- P pulmonale
- S1, S2, S3 pattern = far right axis deviation
- ST segment depression/T wave inversion in anterior/inferior leads
A few discussion points about the diagnostic and supporting criteria. QRS needs to be <120 so that we don’t attribute findings 2/2 RBBB.
A common misconception is to expect a rightward axis deviation (RAD) in RBBB, but in isolated RBBB, the cardiac axis is unchanged; left ventricular activation proceeds normally via the left bundle branch. Generally you would see RAD in bi-fascicular block with RBBB along with left posterior hemiblock. May also see RAD acute right heart strain, lateral MI.
7mm is the number to remember. In RVH, you should see a dominant R in V1 >7mm and a dominant S in V5/V6 >7mm. These numbers reflect the increased myocardial mass of the right ventricle. The persistent S waves in the lateral leads also suggest a clockwise rotation of the heart.
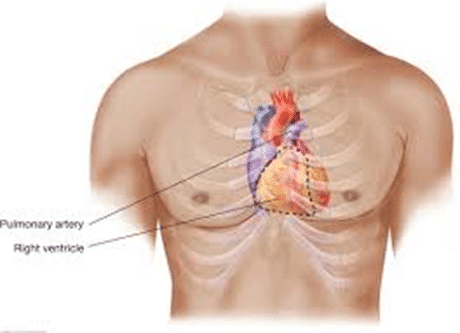
Remember where the right ventricle is in the chest. With RVH, depolarization forces will be directed inferiorly and anteriorly…. BUT, EKG is not sensitive for RVH as most depolarization forces are masked by LV depolarization (generally, mass of L ventricle >R ventricle). So in mild RVH, EKG will appear normal.
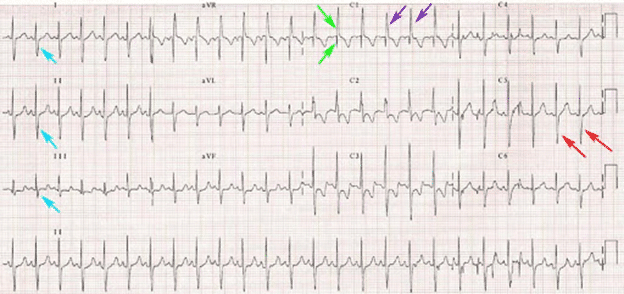
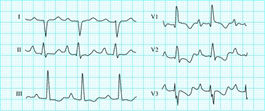
This Pediatric EKG of a 2yo s/p closure of ASD showcases many signs of RVH.
- Blue arrows: S1, S2, S3
- Green arrows: QR in V1
- Purple arrows: >7mm
- Red arrows: Deep S >7mm, also R:S ratio <1
- Possible P pulmonale in lead 2
- Strain pattern in anterior leads
P pulmonale reflects right atrial enlargement, and similar to RVH, is a structural change 2/2 a chronic process.
- Diagnostic criteria for p pulmonale6:
- >/= 2.5mm in lead II
- >/= 1.5mm in V1
Image 6.
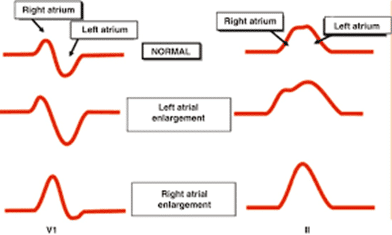
Of note, you would expect a NORMAL PR duration in p pulmonale/RAE. This is because R atrial activity occurs before L atrial activity. The increased R atrial activity duration has greater overlap, but without overtaking, the L atrial activity duration. Contrast this to LAE where PR duration is generally increased (>110-120ms).
Pop board question!: When would you see isolated RAE (w/o RVH)?
Answer: Tricuspid stenosis! Generally we see RAE in association with RVH due to downstream effects. But if there is an obstruction between the RA and the RV as in tricuspid stenosis, then the RA sees greater pressure but the RV does not.
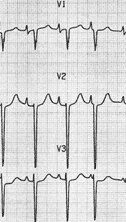
Here is an example of prominent p pulmonale
Image 7.
Notice that this fulfills the diagnostic criteria with >2.5mm in lead 2Image 8.
This shows >1.5mm in lead V1 which is c/w p pulmonale.
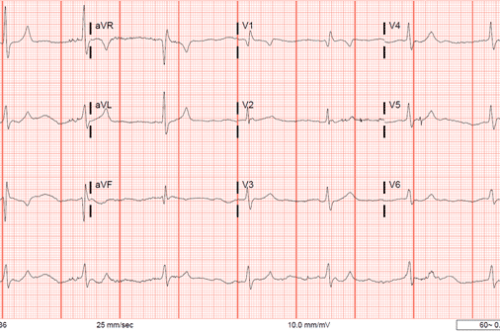
Acute R ventricular strain pattern will be reflected in the anterior and inferior leads (remember positioning of the right heart in the chest). One would expect repolarization disturbances such as ST and T wave changes.
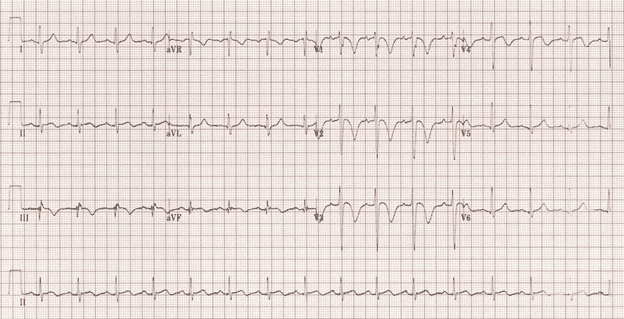
The above EKG is from a pt with acute PE w/ acute R ventricular dilation. Notice the strain pattern in the precordial and inferior leads. Also notice that although the right heart is feeling strain, there are not as many signs for the chronic process of RVH such as tall R waves in V1 or deep S waves in V5/V6.
You see deep and pretty symmetric TWI in the anterior leads, so why is this not Wellens? As discussed on Dr. Smith’s EKG blog7, negative T waves in III and V1 is more specific for PE than ACS (Kosuge et al 2007)8, 99% specific for PE. Only observed in 1% ACS. ACS is unlikely associated with tachycardia. R heart strain more predictive of severity of pHTN 2/2 PE.
Below is a side by side comparison of acute vs chronic right heart strain aka cor pulmonale
Image 10. Image 11.
Image 11 – Example of RVH 2/2 pulm stenosis with strain pattern in anterior leads (ST depressions and T inversions). Dominant R in V1. ?RAE, p wave about 2.5mm in lead 2. RAD
EKG findings in PEs9
- Sinus tachycardia (44%)
- Strain pattern: T wave inversion in the right precordial leads +/- inferior leads (34%), more specific with both
- Nonspecific ST/T wave changes in up to 50%
- S1, Q3, T3 pattern (20%)
- Right bundle branch block (incomplete or complete) (18%)
- Right axis deviation (16%)
- P pulmonale (9%)
- Atrial flutter or fibrillation (8%)
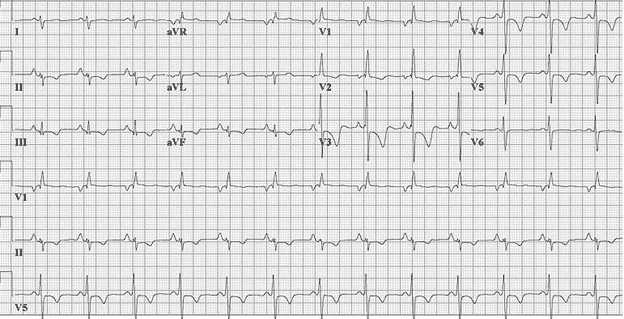
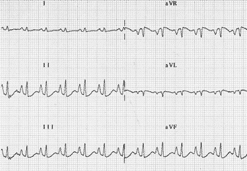
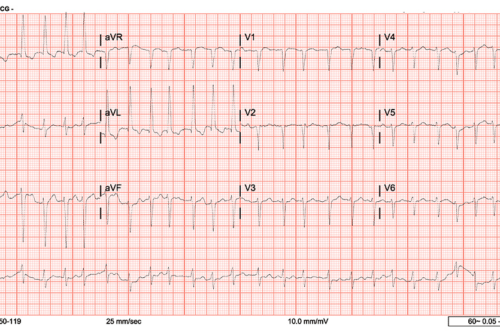
Another example of chronic Pulm HTN. RVH (tall R in V1, deep S in V5/V6). RAE (P pulmonale in inferior leads). Strain pattern- T wave inversions in inferior and anterior leads (v2-v5)
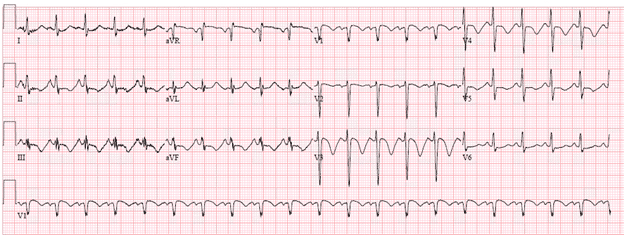
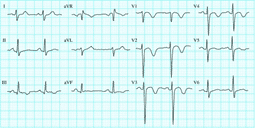
Another PE example. Tachycardia with acute strain pattern in inferior and precordial leads
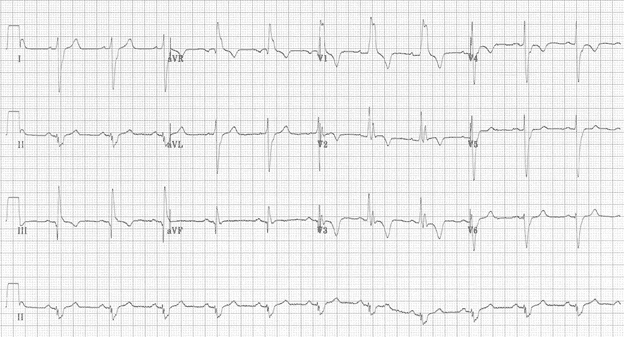
This pt had a massive PE. But there is R >7mm in V1 and S>7mm in lateral leads, and RAD…so is this RVH? Probably not. What we see is RBBB, Classic S1Q3T3 pattern, T wave inversions in V1-V4. Remember that RBBB can be a finding in acute right heart strain and that diagnostic criteria for RVH is QRS <120ms so that RVH characteristics aren’t 2/2 a right fascicular block.
In summary,
- Acute RH strain = ST/T wave changes
- RVH and RAE = signs of chronic structural changes
- Beware of challenge of diagnosing RVH in setting of RBBB
- EKG findings should be used as another data point but are not sensitive nor specific in acute or chronic cor pulmonale!
References
- https://www.uptodate.com/contents/treatment-of-pulmonary-arterial-hypertension-group-1-in-adults-pulmonary-hypertension-specific-therapy?search=pulmonary%20hypertension&source=search_result&selectedTitle=2~150&usage_type=default&display_rank=2https://www.ncbi.nlm.nih.gov/books/NBK499876/
- https://litfl.com/pulmonary-hypertension-echocardiography/
- Price LC, Wort SJ, Finney SJ, Marino PS, Brett SJ. Pulmonary vascular and right ventricular dysfunction in adult critical care: current and emerging options for management: a systematic literature review. Critical care (London, England). 14(5):R169. 2010.
- https://litfl.com/right-ventricular-hypertrophy-rvh-ecg-library/
- https://litfl.com/right-atrial-enlargement-ecg-library/
- http://hqmeded-ecg.blogspot.com/2018/03/a-crashing-patient-with-abnormal-ecg.html
- Kosuge et al. Electrocardiographic differentiation between acute pulmonary embolism and acute coronary syndromes on the basis of negative T waves. Am J Cardiol. 2007 Mar 15;99(6):817-21. [PMID 17350373]
- https://litfl.com/ecg-changes-in-pulmonary-embolism/
- https://litfl.com/pulmonary-hypertension/
Images
- My patient’s CXR, HIPPA protected
- https://litfl.com/wp-content/uploads/2018/08/ECGH-RVH-Right-ventricular-hypertropy-RV-Strain.jpg
- https://phassociation.org/wp-content/uploads/2017/02/who-group-infographic.jpg
- https://encrypted-tbn0.gstatic.com/images?q=tbn%3AANd9GcTK8AN-uyX0vkiTU_jNd4bTL_kzYEXt6pmit6IY8QRKCHMum7jn
- http://www.metealpaslan.com/ecg/v/000082-01v.jpg
- https://encrypted-tbn0.gstatic.com/images?q=tbn%3AANd9GcQvlu3yl3p5wmmp-_gsBcoUi6-1NVoJVS5voiMKUtcUArfunnHr
- https://litfl.com/wp-content/uploads/2018/08/ECG-Peaked-P-waves-P-pulmonale-RAH.jpg
- https://litfl.com/wp-content/uploads/2018/08/P-pulmonale-Right-atrial-hypertrophy-in-V1-V2.jpg
- https://litfl.com/wp-content/uploads/2018/08/ECG-Massive-Pulmonary-embolus-RVH-RV-Strain.jpg
- https://europepmc.org/articles/PMC1123164/bin/ecg12.f6b.jpg
- https://europepmc.org/articles/PMC1123164/bin/ecg12.f2.jpg
- https://www.wikidoc.org/images/b/bb/Pulhtn1.jpg
- https://4.bp.blogspot.com/-hN61nJ8hQlE/WqFeKD5PqJI/AAAAAAAAA_Q/T9_DalLeE5IzcxAdJCn7rmXye0yfwDScwCEwYBhgL/s1600/acute-rv-strain_presentation.png
- https://litfl.com/wp-content/uploads/2018/08/ECG-Massive-bilateral-pulmonary-embolus-2.jpeg
All image references and credits due to originals authors.

This Post Has 0 Comments